Non-Scalpel Vasectomy
Non Scalpel Vasectomy performed by Dr. Kelanda-Sedra in Niagara Falls, ON
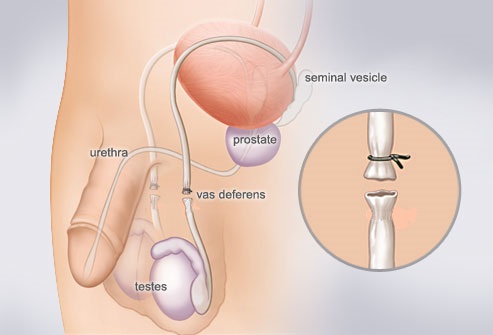
What is a vasectomy?
Vasectomy is a permanent male contraceptive method. It is done as an outpatient procedure under a long-acting local anesthetic that lasts for 8 hours. This along with the protocol of Tylenol & Ibuprofen as anti-inflammatory medication makes the procedure comfortable.
The vas deferens – the duct that transports the sperm to the ejaculatory ducts-is isolated, cut & blocked so that it can no longer transport sperm in the ejaculate. Thus, the man becomes permanently infertile. Recanalization is extremely rare 1in 40,000-50,000. The patient embarking on the procedure should consider it irreversible. There are reversible procedures available but they are not covered by OHIP benefits so they can be costly and are not 100% effective.
How is Vasectomy Performed ?
The procedure that is employed in this office is “No-Scalpel Vasectomy”. In most instances one can isolate the vas deferens through a tiny hole on the scrotum. Then it is tied on one end and a 1 cm segment is cut off, the other end is then buried. This is done so that the two ends of the tube do not rejoin to create a new duct that will transport sperm causing failure of the procedure. There are no sutures required to the skin of the scrotum. The no-scalpel vasectomy is also known as “Gentle Vasectomy”. As the name implies, it is more gentle with lowered incidence of infection and bleeding or hematoma. In this office “Traditional Vasectomy” is reserved for difficult scrotal anatomy whether due to prior surgery or under-developed extremely short neck scrotum. The doctor does examine the patient upon consultation and this is explained to the patient at the consultation time.
Myths about Vasectomy:
Myth #1 Vasectomy lowers the libido due to reduced testosterone
Vasectomy does not lower testosterone, or impact sex drive. If anything there is more freedom in intimacy because the fear of conception has been eliminated. The testicle continues to secrete testosterone through the Leydig cells under the brain’s command through the hypothalamic-pituitary instruction pathway
Myth #2: Vasectomy causes Erectile Dysfunction or interferes with ejaculation
There is no erectile dysfunction as a result of vasectomy. Both libido and ejaculation are unhindered in any way. The patient will maintain his pre-vasectomy functional abilities. Ejaculatory fluid comes mostly from the prostate and seminal vesicle, only a tiny amount from the testicle.
Myth #3: Vasectomy can cause prostate cancer
Vasectomy does not induce or cause prostate cancer. When you are under the care of a physician that screens for prostate cancer the coincidence of detection is higher than if you do not check with a physician. There is no cause-effect from the vasectomy. The absence of the sperm does not lead to cancer. The testosterone hormone is still excreted the same as pre-vasectomy. Sperm continues to be produced by the testicle but is not transported to the prostatic urethra and ejaculatory tubes. These untransported sperm eventually die and are reabsorbed by the body.
Myth #4 Tubal ligation is easier than vasectomy
This myth is easily dispelled. Testicles are in the scrotum, which is literally hanging outside of the body. A woman’s fallopian tubes are found deep inside the pelvis. A vasectomy requires cutting the skin of the scrotum and vas deferens. It is performed with local anesthetics. Tubal ligation requires a very complicated surgical procedure that opens the skin, goes through the fatty tissue, the muscle tissue, and the peritoneum. After reaching the pelvis, doctors need to locate the tubes and block them. Such a complex procedure requires general anesthesia or epidural anesthesia.
Post-operative complications represent another issue. Vasectomy complications are infrequent. Patients need to be careful and report symptoms such as fever or changes in the wound. Tubal ligation recovery is often completed as an inpatient in a hospital or clinic. Women need very close follow-up, and the risk of infection, bleeding, and other complications are higher.
Myth #5. You can promptly resume sex after vasectomy
Vasectomy is an outpatient procedure but requires a recovery time of around one week. During this week, you need to avoid physical exercise, working or sitting for too long, and having sex. You can’t have sex during the first week or a few days. Follow the instructions given by the doctor, and if you still feel pain after resuming sexual activity, wait a few extra days.
Myth #6: You are instantly sterile after a vasectomy
The birth control effects of vasectomy are not immediate. If a patient starts having unprotected sex right after vasectomy, pregnancy can occur. You will be required to provide samples for sperm count tests to make sure that the procedure was effective. It will be one week without sex and around three months using additional contraceptives before results are certain.
Myth #7: Condoms are no longer required after vasectomy
As noted above, you may need condoms for a while after vasectomy, even with a stable partner. Keep in mind that vasectomy only works to avoid pregnancies. It does not protect you from sexually transmitted diseases. Transmission only requires skin-to-skin contact or fluid contact, depending on the disease. Doctors recommend against unprotected sex, vasectomies do not make an exception.
Myth #8. Vasectomy is always an irreversible procedure
Vasectomies are designed to be irreversible and cause male infertility. That’s why doctors will ask many questions and make sure that you don’t want to get anyone pregnant in the future. However, some cases can be reversed without a guarantee. The capacity to reverse your vasectomy depends on the type of vasectomy you got and the time since. In some cases, your organism develops antibodies against sperm cells after a vasectomy. If that happens in your case, it will compromise the capacity to reverse the procedure.
If you’re worried about having an irreversible procedure, vasectomy is probably not the best birth control for you. Talk to your doctor if you are having doubts, or prefer a truly reversible birth control method. Other vasectomy alternatives include condom use, non-penetrative sexual intercourse, intrauterine devices, implantable skin devices, and more.
Call the office to book a consultation. This procedure is covered by OHIP
Contact Us Today
For More Information about Acne Treatments, or to schedule an appointment, call us at
(905) 937-9559 or click the button below to contact us online
